
Your jaw is an amazing part of your anatomy. The jaw bone (your mandible) sits in a small fossa (or depression) in the temporal bone of your skull. This is why you may have heard of it called the “TMJ”, its other name is the temporomandibular joint. Pain in this part of the face (i.e. not teeth or headache related) is usually referred to as TMD (temporomandibular disorder).
How common is jaw pain (TMD)? And what other pain do you have?
Jaw pain is not as common as low back pain or headache but Dutch and German studies from 2015 placed jaw pain as occurring in between 4 to 8 % of the general population. One point of interest was that the studies disagreed on the role gender played in jaw pain. One study showed jaw pain was somewhat more common in females; the other showed no statistical difference between the genders. It’s been suggested that jaw pain is more prevalent in young adults and that it declines after middle age but the Dutch study looking at age prevalence felt there was insufficient evidence to support that.
The most interesting finding from both papers was that almost everyone who was asked, had pain in other areas of their body. The most common being, back pain, neck pain and headache.
I’ve written an earlier blog about how your jaw might be causing your headache, you can read it here, so it’s interesting to consider, do people who seek treatment for other symptoms, like headache or neck pain, neglect to mention their jaw pain? I know I always ask my patients with headache or neck pain whether they have jaw pain.

What are the risk factors for jaw pain?
The most obvious risk factor is trauma like a direct blow to the jaw, but trauma also includes whiplash injuries and opening the mouth for a long period of time as in extensive dental work. Oral habits like clenching the jaw, chewing gum or grinding your teeth (bruxism) contribute to the load on the jaw joint.
Poor posture can also contribute to jaw pain because if your head sits forward see (picture below) the jaw naturally drops opens and so the jaw muscles have to work all day. Other factors include your dental bite, stressful life events and emotional factors. Your osteopath will take stock of these factors when treating your jaw pain.
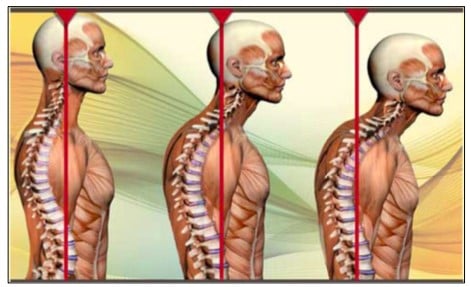
So, how does the jaw work?
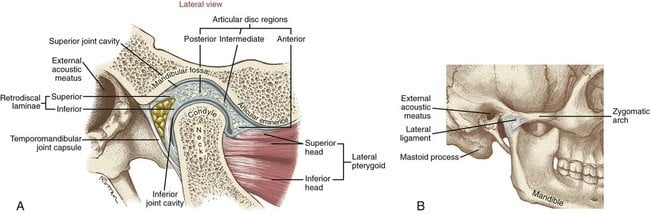
The TMJ is like your shoulder joint in the sense that the bones don’t make much of the joint, it’s the capsule, ligaments and muscles around it (see picture below) that give it the structure that makes it work so well – until it doesn’t. The jaw is also different because there is a soft disc between the 2 bones to keep the bones moving smoothly while you open and close your jaw.
When you open your mouth; to eat, to talk or sing, for example, the jaw-bone moves forward and down (protrusion and depression, in medical terms) in relation to your skull to enable maximum, pain free and stable movement. It’s these structures that your osteopath will investigate to ensure a focussed and effective treatment.
Seeing your local osteopath can help to reduce symptoms of jaw pain and the side effects of poor posture, jaw clenching and teeth grinding. We’ll assess your jaw (TMJ), neck and shoulders as each of these areas can contribute to jaw pain. Inter-oral techniques, which are very effective, may also be utilised to help alleviate jaw tightness and headache symptoms.
As Osteopaths we are experienced in assessing your posture; and will ascertain whether this is a factor in your jaw pain. We will also prescribe some stretching or massage techniques that you can do at home to help with the symptoms of jaw pain.
If you feel like you may suffer from jaw pain, why not give us a call today and find out how we can help!




